 Model 3 exhibited the thinnest mid-myocardium and thickest epicardium and endocardium. Model 2 had intermediate layer thicknesses. We used a computational method and simulated three heterogeneous ventricular models: Model 1 had the thickest M cell layer and thinnest epicardium and endocardium. The objective of this study was to observe the effects of different thickness ratios of the epicardium, mid-myocardium, and endocardium on cardiac arrhythmogenesis, reentry instability, and mechanical responses during arrhythmia.  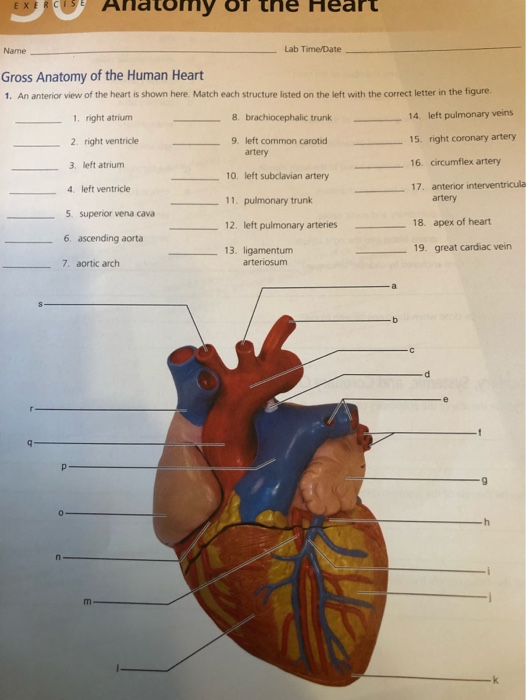
Therefore, this results in possible variations in the heterogeneity ratios between the epicardium, mid-myocardium, and endocardium. However, the wide variability of myocardial shapes and the unclear edges between the epicardium and soft tissues are major challenges in the 3D model segmentation approach for identifying the boundaries of the epicardium, mid-myocardium, and endocardium. Construction of an accurate three-dimensional (3D) model of the heart is important for predicting physiological behaviors. As indicated by preliminary studies, heart-wall layers exhibit various characteristics with regard to electrophysiology, pharmacology, and pathology. Among these layers, the mid-myocardium is typically the thickest. 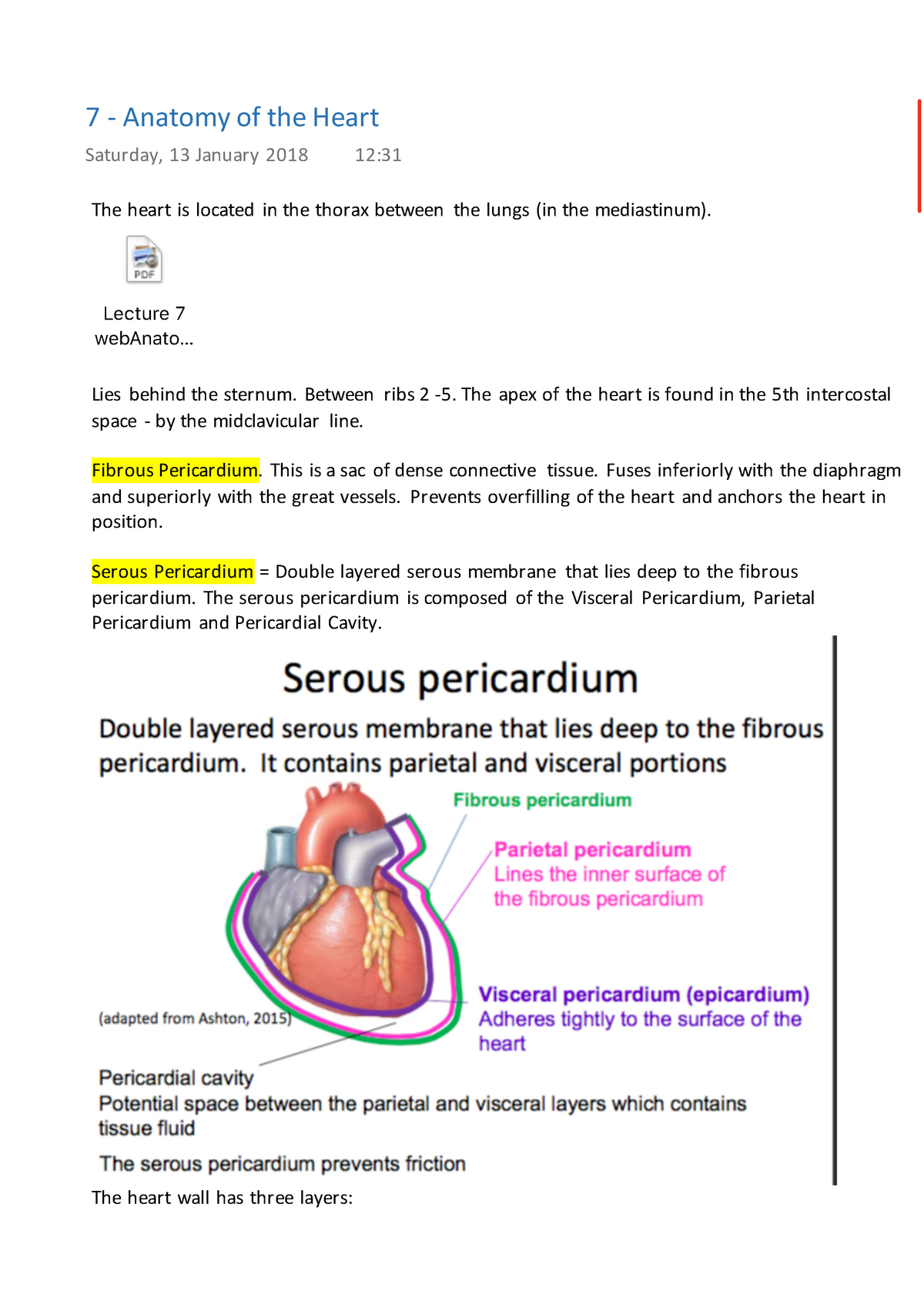
The papillary muscles contract during ventricular contraction and generate tension on the valve leaflets via the chordae tendineae to prevent the AV valves from bulging back into the atria and becoming incompetent. The semilunar valves (pulmonic and aortic) do not have analogous attachments.The heart wall exhibits three layers of different thicknesses: the outer epicardium, mid-myocardium, and inner endocardium. Tricuspid and mitral valves (also called atrioventricular, or AV valves) have fibrous strands ( chordae tendineae) on their leaflets that attach to papillary muscles located on the respective ventricular walls. When the LV contracts, it expels blood through the semilunar aortic valve and into the aorta, which then distributes blood to the arterial system. The LV wall is very thick so that it can generate high pressures when it contracts (normally ~120 mmHg at rest). Blood flows from the LA, across the mitral valve, and into the left ventricle (LV). This chamber is similar to the RA because it is very distensible, although the blood pressure within the LA is several mmHg higher than the RA (6-10 mmHg in the LA compared to 0-3 mmHg in the RA). Blood returns to the heart from the lungs through four pulmonary veins that enter the left atrium (LA). 
The pulmonic valve, like all healthy heart valves, permits blood to flow in only one direction. As the RV contracts and generates pressure, blood leaves the RV, flows across an open semilunar pulmonic valve, and enters the pulmonary artery that distributes the output of the right ventricle to the lungs where exchange of oxygen and carbon dioxide occur. The free wall of the right ventricle is not as thick as the left ventricle, and anatomically, it wraps itself around part of the larger, and thicker, left ventricle. The RV wall, however, is thicker and more muscular than the RA, so that when it contracts, it can develop considerably more pressure (~25 mmHg) than the RA. Blood passes from the RA to the RV through the tricuspid valve. It also undergoes spontaneous contractions (see cardiac cycle) to aid in the filling of the right ventricle (RV). Because of its high compliance, the RA pressure is normally very low (0-3 mmHg). The right atrium has a relatively thin muscular wall and easily expands with blood as it fills (i.e., it is highly compliant). Venous blood enters the right atrium (RA) of the heart through the superior vena cava (SVC) and inferior vena cava (IVC). 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
